
Imagine waking up every day with itchy, painful patches of red, scaly skin—and never knowing when they’ll get better or worse. For millions of people, this isn’t just a bad skin day—it’s psoriasis, a chronic autoimmune condition that affects far more than appearance. With its unpredictable flare-ups and emotional toll, psoriasis can interfere with daily life, relationships, and self-esteem.
In this article, we’ll explore what psoriasis is, what causes it, how it’s treated, and what new research is revealing about this often misunderstood condition. Whether you’re newly diagnosed or seeking to support someone living with it, understanding psoriasis is the first step toward better care—and better quality of life.
What Is Psoriasis?
Psoriasis is a chronic (long-lasting) skin disorder marked by scaling and inflammation, affecting approximately 2 to 2.6 percent of the U.S. population—or about 5.8 to 7.5 million people. Although it can appear at any age, it most commonly develops in adults and affects males and females equally.
The disease occurs when skin cells rise rapidly from their origin below the skin’s surface and accumulate before they fully mature. Typically, this skin cell turnover process takes about a month, but in psoriasis, it can happen in just a few days. As a result, psoriasis typically manifests as thick, red, inflamed patches of skin covered with silvery scales.
These patches, often referred to as plaques, are usually itchy or painful. They commonly appear on the elbows, knees, legs, scalp, lower back, face, palms, and soles of the feet—but can develop anywhere on the body. Psoriasis can also affect the fingernails, toenails, and soft tissues of the genitals and mouth.
In some cases, the skin around joints may crack. Additionally, about 1 million people with psoriasis experience joint inflammation that leads to arthritis-like symptoms, a condition known as psoriatic arthritis.
How Does Psoriasis Affect Quality of Life?
Psoriasis can significantly impact a person’s physical and emotional well-being. Persistent itching and pain may interfere with basic activities such as self-care, walking, or sleeping. Plaques on the hands or feet can limit occupational capabilities, recreational activities, and caregiving responsibilities.
The burden of ongoing medical care is not only costly but can also disrupt work or school schedules. People with moderate to severe psoriasis often report low self-esteem, body image issues, and social anxiety due to their appearance. These emotional challenges may lead to depression and social withdrawal.
RELATED: 5 Psoriasis Treatments Black Sufferers Should Avoid
What Causes Psoriasis?
Psoriasis is an immune-mediated condition primarily involving T cells, a type of white blood cell responsible for defending the body against infections. In psoriasis, T cells are mistakenly activated and become hyperactive, setting off a chain of immune responses that accelerate skin cell production and inflammation.
Genetics plays a role: about one-third of people with psoriasis have a family history of the condition. Researchers have identified specific genes associated with psoriasis, highlighting the hereditary component.
Flare-ups may be triggered by a variety of external factors, including:
-
Infections (especially strep throat)
-
Stress
-
Cold, dry climates
-
Certain medications (such as lithium and beta-blockers)

How Is Psoriasis Diagnosed?
Diagnosing psoriasis can be challenging because it often resembles other skin conditions. A dermatologist may need to examine a small skin biopsy under a microscope to confirm the diagnosis.
There are several types of psoriasis, including:
-
Plaque Psoriasis: The most common type, characterized by raised, red lesions with silvery scales.
-
Guttate Psoriasis: Small, drop-shaped spots typically appearing on the trunk, limbs, and scalp, often triggered by upper respiratory infections.
-
Pustular Psoriasis: Blisters filled with noninfectious pus, often brought on by stress, infections, or medications.
-
Inverse Psoriasis: Smooth, bright red patches in skin folds (e.g., under breasts, around genitals, or in armpits), aggravated by friction and sweat.
-
Erythrodermic Psoriasis: A severe form involving widespread redness and shedding of the skin, possibly caused by sunburn, medications, or uncontrolled psoriasis.
-
Psoriatic Arthritis: Joint inflammation occurring in patients with, or who later develop, psoriasis.
RELATED: 6 Psoriasis Self-Assessment Tools Black People Need to Know About
How Is Psoriasis Treated?
Treatment for psoriasis is tailored based on the severity of the disease, the type of psoriasis, and the patient’s response to previous therapies. Doctors often follow a “1-2-3” treatment approach:
-
Topical treatments: Applied directly to the skin.
-
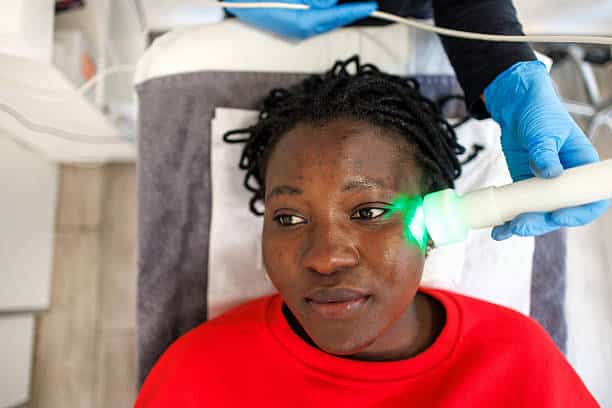
Phototherapy: Exposure to ultraviolet light.
-
Systemic therapy: Oral or injected medications that target the immune system.
Over time, treatments may lose effectiveness, particularly topical corticosteroids, which can lead to skin thinning and other side effects. Because patient response varies, treatment often requires trial and error, and therapies may be rotated every 12 to 24 months.
Topical Treatments
Applied directly to the skin, topical therapies are often the first step in treatment. These include:
-
Corticosteroids: These reduce inflammation, slow down skin cell turnover, and suppress immune activity. Available in various strengths, they are usually applied twice daily. Potent corticosteroids may be used for stubborn plaques or areas with limited skin involvement. Milder preparations are preferred for sensitive areas like the face or genitals. Long-term use should be monitored to avoid side effects such as thinning skin or resistance.
-
Calcipotriene: A synthetic form of vitamin D3












