
If there is one common thread among the “Health Warriors” of the Black community—those navigating heart disease, kidney conditions, or rare illnesses—it is the fundamental desire to be seen by the healthcare system. For too long, Black Americans, who represent 13% of the population, have been sidelined in the research and clinical guidance that directly determine their survival.
To bridge this systemic gap, BlackDoctor and USA TODAY recently met in New York City for their third annual summit. Guided by the theme “Generational Health: Blueprint for Longevity,” the event gathered hundreds of industry leaders, medical experts, and advocates to move past “business as usual” and architect real-world solutions for the community.
To watch the panels, click on the hyperlinked titles listed below.
The summit opened with Jenny Huang (Director, B2B Brand Marketing, USA TODAY) and Kristin Vaughan (Chief Content Officer, BlackDoctor). Their premise shared an absolute: there is no medical progress without foundational trust.


“We aim to provide guidance that makes complexities clear,” Vaughan shared. “Our community trusts us to provide data and studies through a ‘how-to’ lens while emotionally connecting through shared lived experiences.”
The day’s tone was further shaped during a keynote fireside chat with Akinwole (Aki) Garrett (President and COO, BlackDoctor) and Dr. Yele Aluko, MD, MBA (Principal, Aluka Advisors, Health System Performance & Equity Leader). Together, they reframed generational health not as a list of symptoms, but as a systemic challenge, urging the medical community to look at the factors—like access and representation—that determine outcomes across generations.



Equity is not a singular event; it is won through the accumulation of “marginal gains” that transform how care is delivered at the local level. This session explored how small, consistent actions—like utilizing plain language and intentional community outreach—compound into massive, population-level change.
“These aren’t abstract issues. People are dying. Families are navigating systems that too often feel out of reach, inconsistent, or untrustworthy. The stakes couldn’t be higher,” Harville reflected after the event. “What I know for sure is progress will not come from any one institution, sector, or voice. It will take all of us… working in concert to rebuild trust, improve access, and drive lasting change.”
Dr. Megan Wanzo added that what is often labeled as “mistrust” is frequently pattern recognition grounded in lived experience. “Resilience should not be the business model of our healthcare system,” Wanzo shared, calling for a move from episodic care to true community partnership.




Innovation loses its value if it fails to cross the threshold of the communities that need it most. This forward-looking dialogue examined the pivotal turning point where medical teams must prioritize patient accessibility over clinical function.
“Progress isn’t only defined by what we discover; it’s defined by who it reaches,” Dr. Tania Small shared. “Because what good is innovation if it’s not reaching the people who have the disease?”


The silent indicators of kidney disease often go unnoticed until the damage is irreversible, making early education a matter of life or death. Panelists focused on the urgency of “knowing your kidney numbers,” specifically monitoring phosphorus to ensure transplant readiness.
“Kidney health is shaped long before a diagnosis is made; it’s shaped by the information we’re given, the trust we have in the system and the knowledge passed down through our families and lived experiences,” Dr. Williams shared. “Generational health means recognizing that access, awareness and outcomes are often inherited.”



For many living with Hidradenitis Suppurativa (HS), the physical pain of the condition is often rivaled by the psychological weight of a decade-long wait for a correct diagnosis. This intimate “living-room conversation” stripped away the clinical jargon to reframe HS as a deeply human story. By centering the lived experiences of advocates alongside clinical expertise, the panel explored how the combination of public misunderstanding and systemic medical gaslighting creates a profound emotional toll that requires a holistic, community-based approach to healing.
RELATED: From Reactive to Proactive: The Power of Storytelling in Breaking the HS Stigma
“We should not underestimate how much it means for people to be able to tell their stories and to own their stories,” Espy shared.
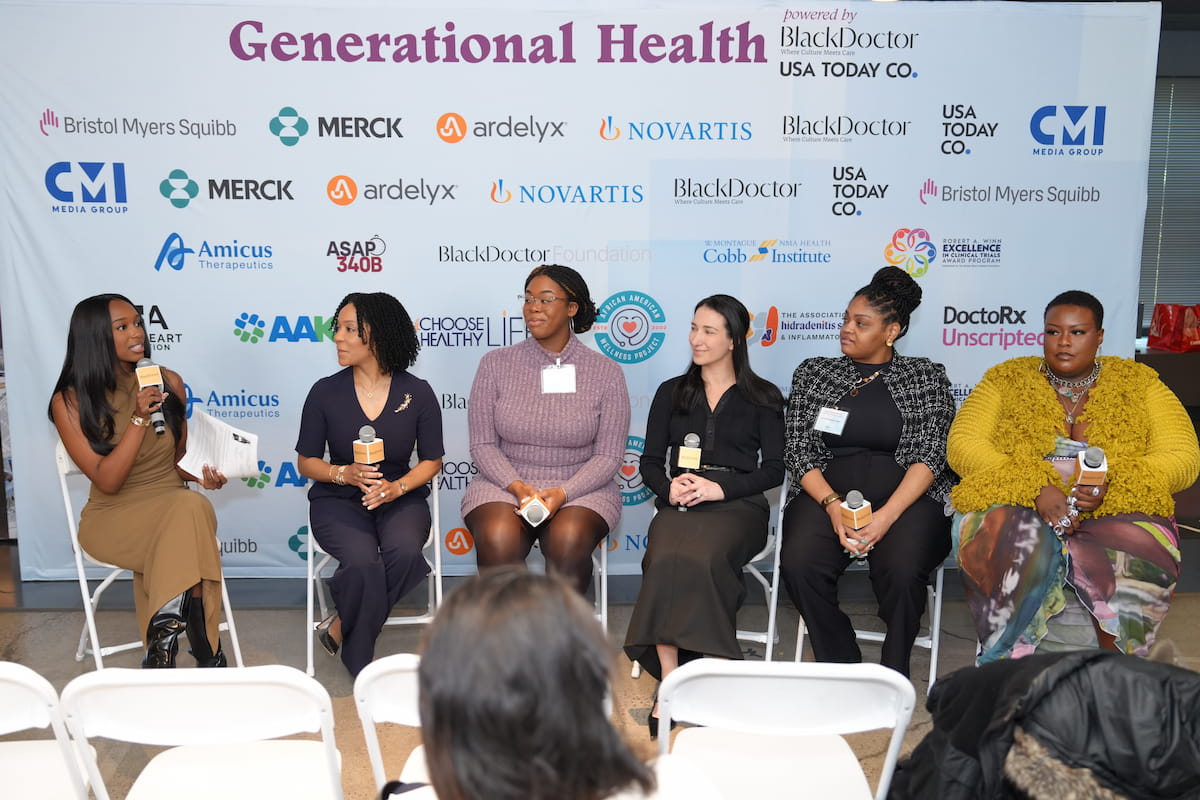



When the financial safety nets intended for the most vulnerable patients lack transparency, the result is a “generational threat” of medical debt that drains the wealth and health of Black families. This sobering dialogue took a hard look at the 340B program, examining the disconnect between the legislative intent of drug discounts and the reality of patients who never see those savings. The panel argued that without radical accountability, these programs risk becoming another systemic barrier rather than the lifeline they were designed to be.
“These are the stories that need national platforms… This is the work I do: showing up for conversations that center patient voices. Building platforms. Speaking truth where it matters,” Barnes noted.
Heart health is more than a personal medical status; it is a vital component of a family’s legacy that must be guarded with clinical precision and collective action. By reframing LDL-C (bad cholesterol) from an abstract metric into a primary indicator of generational longevity, this panel shifted the conversation away from individual blame toward family empowerment. The discussion focused on how “knowing and owning your numbers” provides the necessary leverage to advocate for better care and ensure that heart disease does not remain an inherited burden.




In the fight against cancer, the greatest obstacle to survival is often not the biological complexity of the disease, but the rigid and often exclusionary bureaucracy of the American healthcare system. This panel laid bare the hard truth that medical outcomes are frequently tethered to insurance approvals and administrative gatekeeping. The speakers underscored that for innovation to actually save lives, patients and advocates must be equipped to challenge the status quo and demand a “standard of care” that is both accessible and culturally competent.
“No one cares how great America is if your insurance company says ‘No’!” noted Zachary, highlighting the need for aggressive patient advocacy.


The summit concluded with a focus on the Voices of Black Women initiative, a landmark study by the American Cancer Society. By enrolling Black women in this research, the initiative ensures that the “blueprint for longevity” is built on data that actually represents the community.
In conclusion, the BlackDoctor and USA TODAY Generational Health: Blueprint for Longevity Summit hopes to leave people inspired, more curious and desire to develop actionable solutions and systems for impact.


By subscribing, you consent to receive emails from BlackDoctor.com. You may unsubscribe at any time. Privacy Policy & Terms of Service.